
The University of Iowa
Department of Ophthalmology and Visual Sciences
February 15, 2008
Age-related macular degeneration (AMD) is the most common cause of vision loss in American adults over the age of 60. The presence of drusen within the macula is a common examination finding in patients with AMD. Here we further evaluate the histopathologic charactaristics of drusen in AMD.
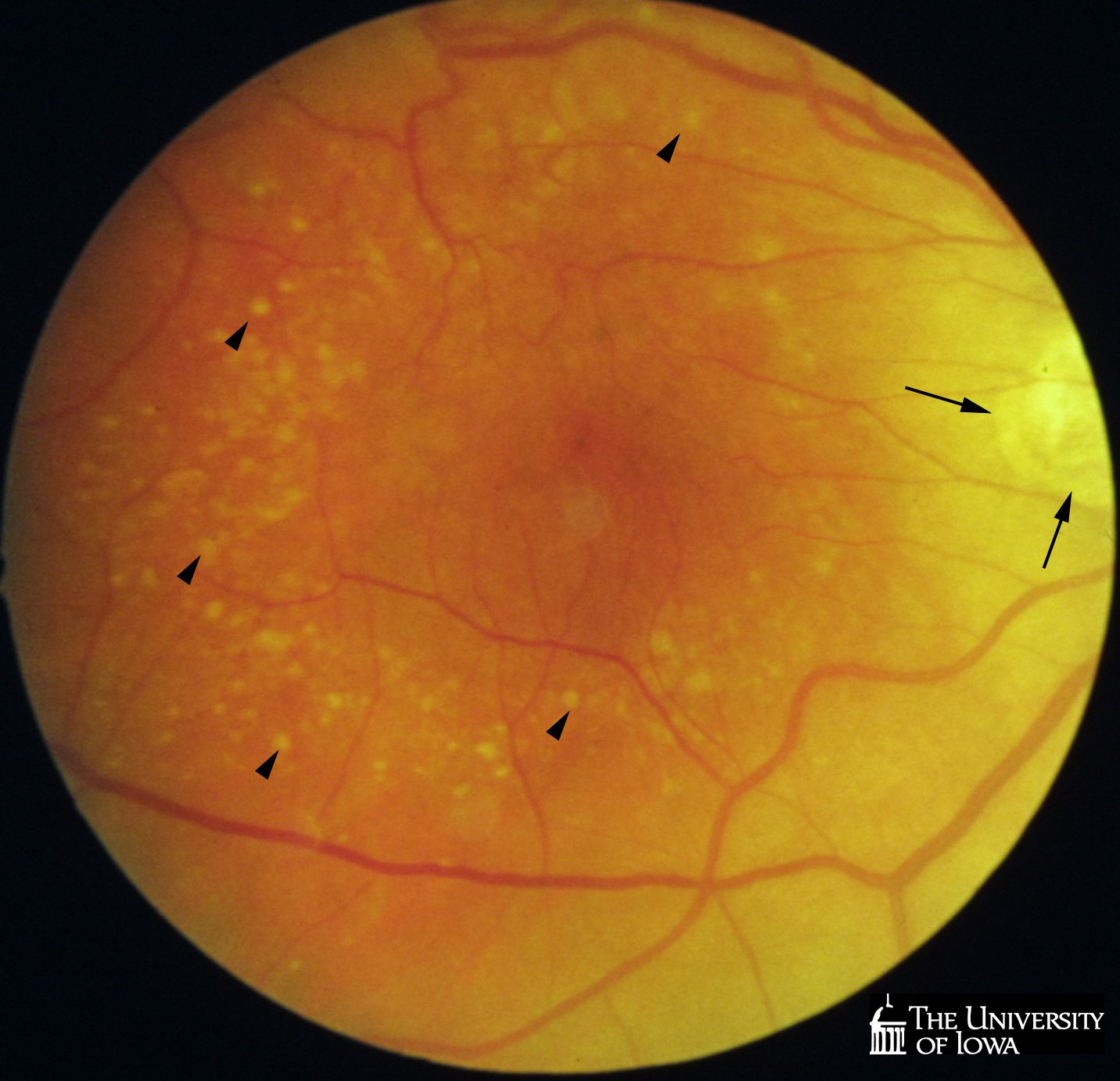
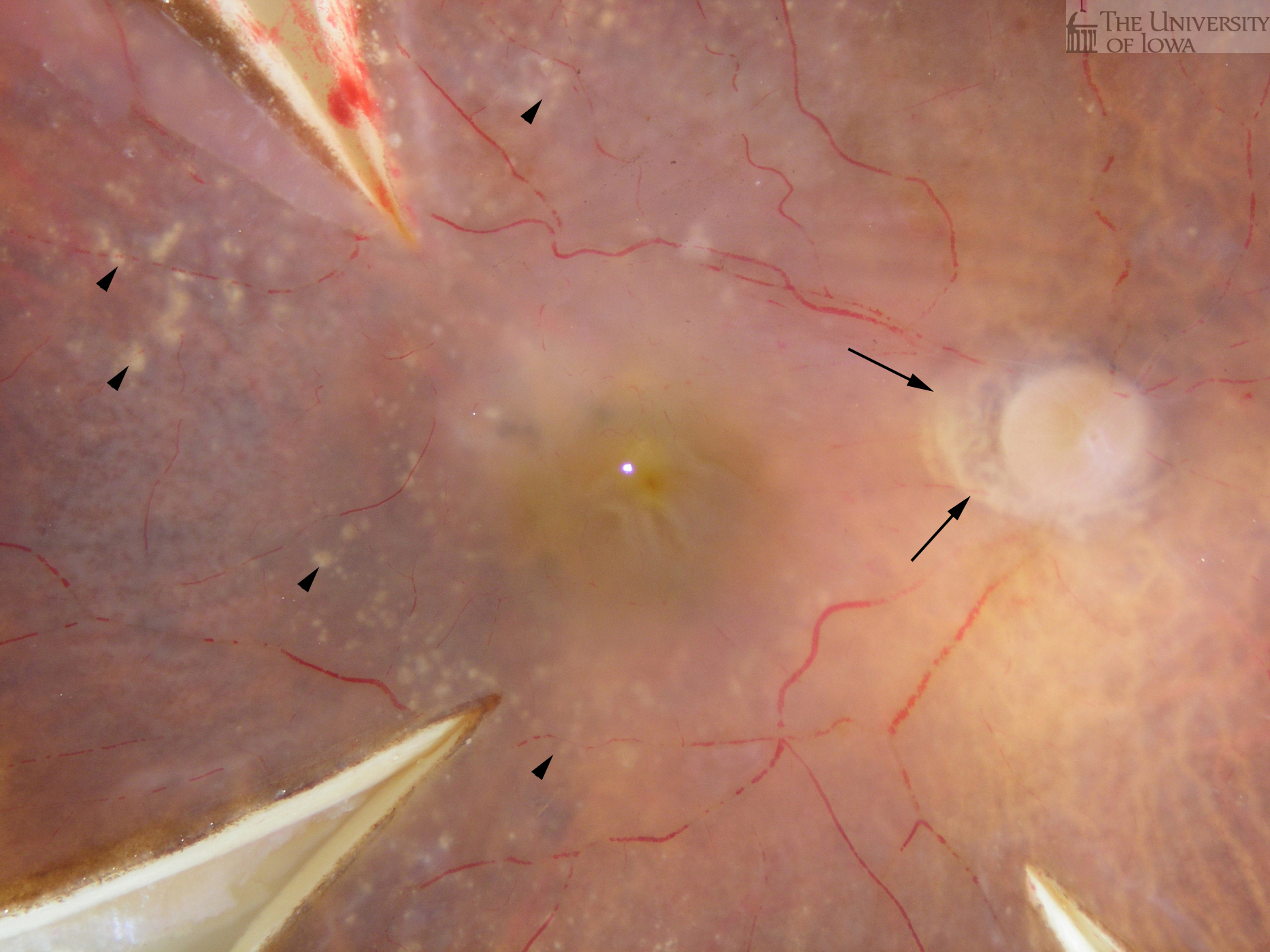
Eyes were obtained for research from an 88-year-old donor following appropriate informed consent. A fundus photgraph, gross photograph and histological sections of the same eye are here depicted. The left eye showed extensive choroidal neovascularization and disciform scarring and is described in a previous report. Note the presence of drusen in an annular pattern (arrowheads) and peripapillary atrophy (arrows) on both fundus and gross photographs (Figures 1A and 1B).
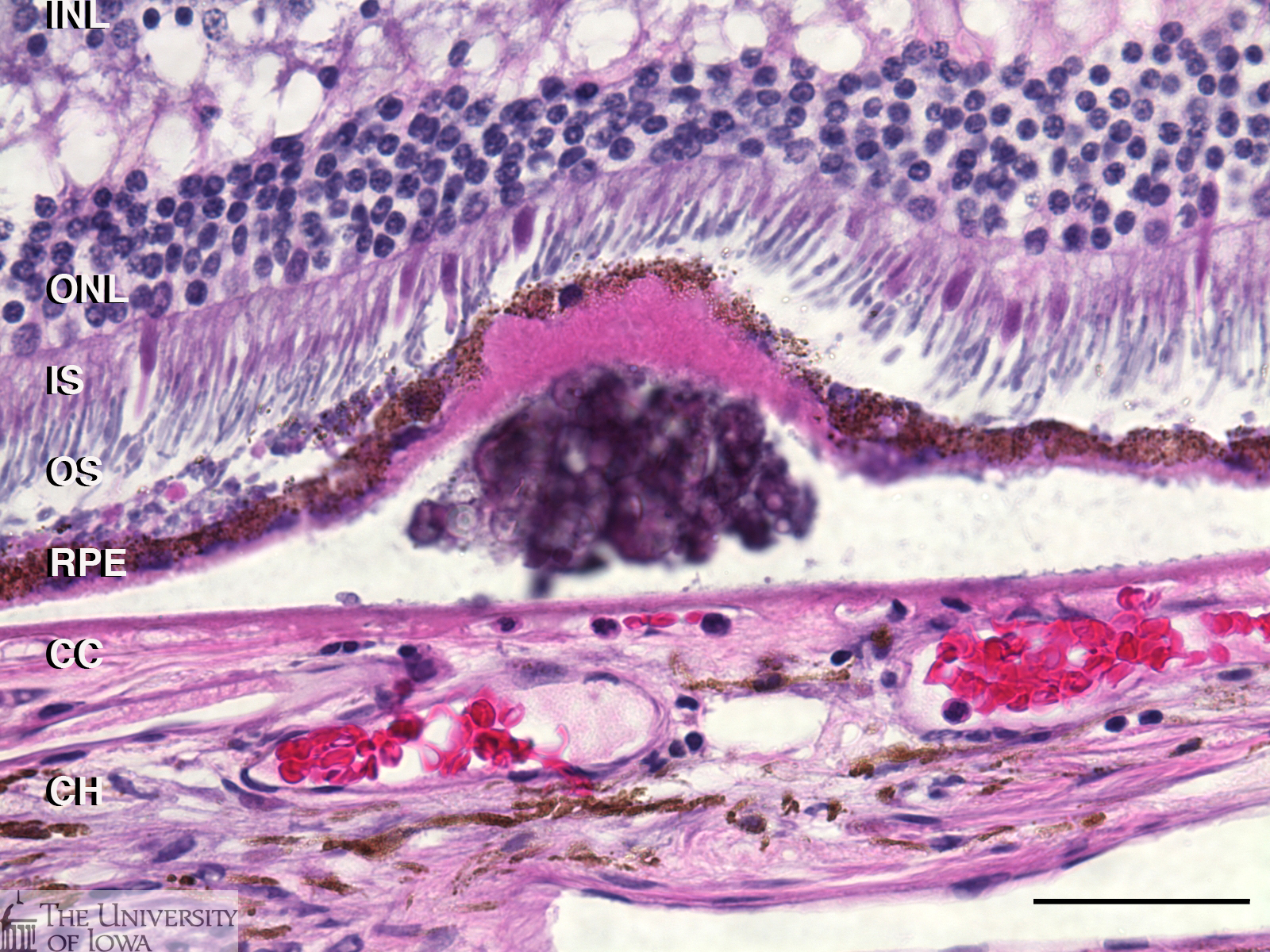
Histological section stained with hematoxylin and eosin shows a sub-RPE deposit from within the ring of drusen. In some cases drusen show substructural organization or layering; note the hematoxylin stained globular material within the deposit (see Figure 2). The attenuation of the retinal outer nuclear layer (ONL) as well as photoreceptor inner and outer segments, is not uncommon. Corresponding changes in gene expression observed in retinal cells overlying drusen has been described.
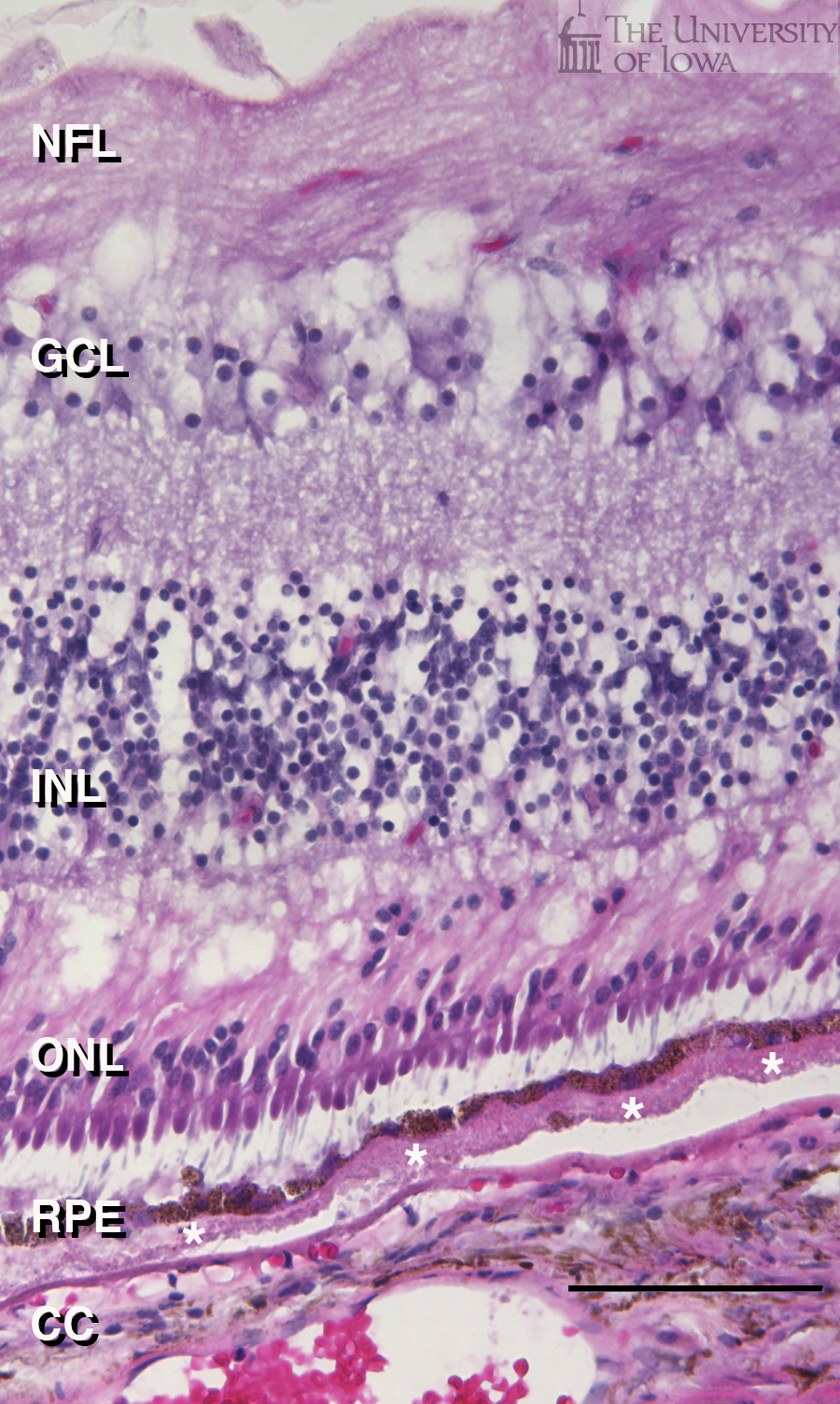
In addition to mounded, spherical or hemispherical deposits, diffuse extracellular deposits (basal laminar deposits or basal linear deposits) are also observed in macular degeneration, and were present in the macula of the same eye (white asterisks, Figure 3).
When examined by fluorescence microscopy, lipofuscin in the RPE is highly autofluorescent when excited with both blue light (green emission) and green light (red emission). Areas of overlap in this merged image appear yellow. In contrast, subRPE deposits and Bruch’s membrane (arrows) show much greater emission over shorter wavelengths and thus appear predominantly green in this merged image (see Figure 4).
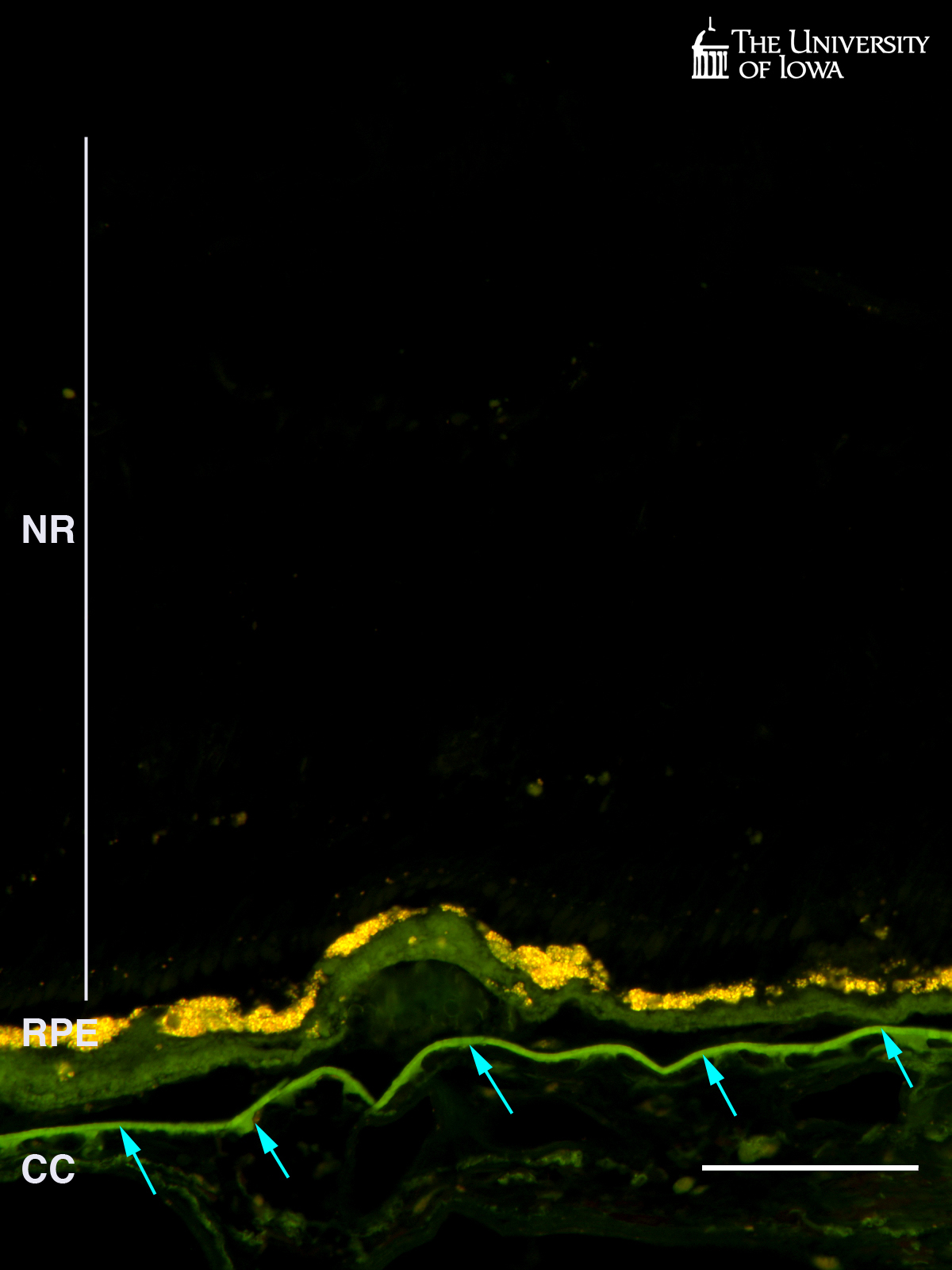
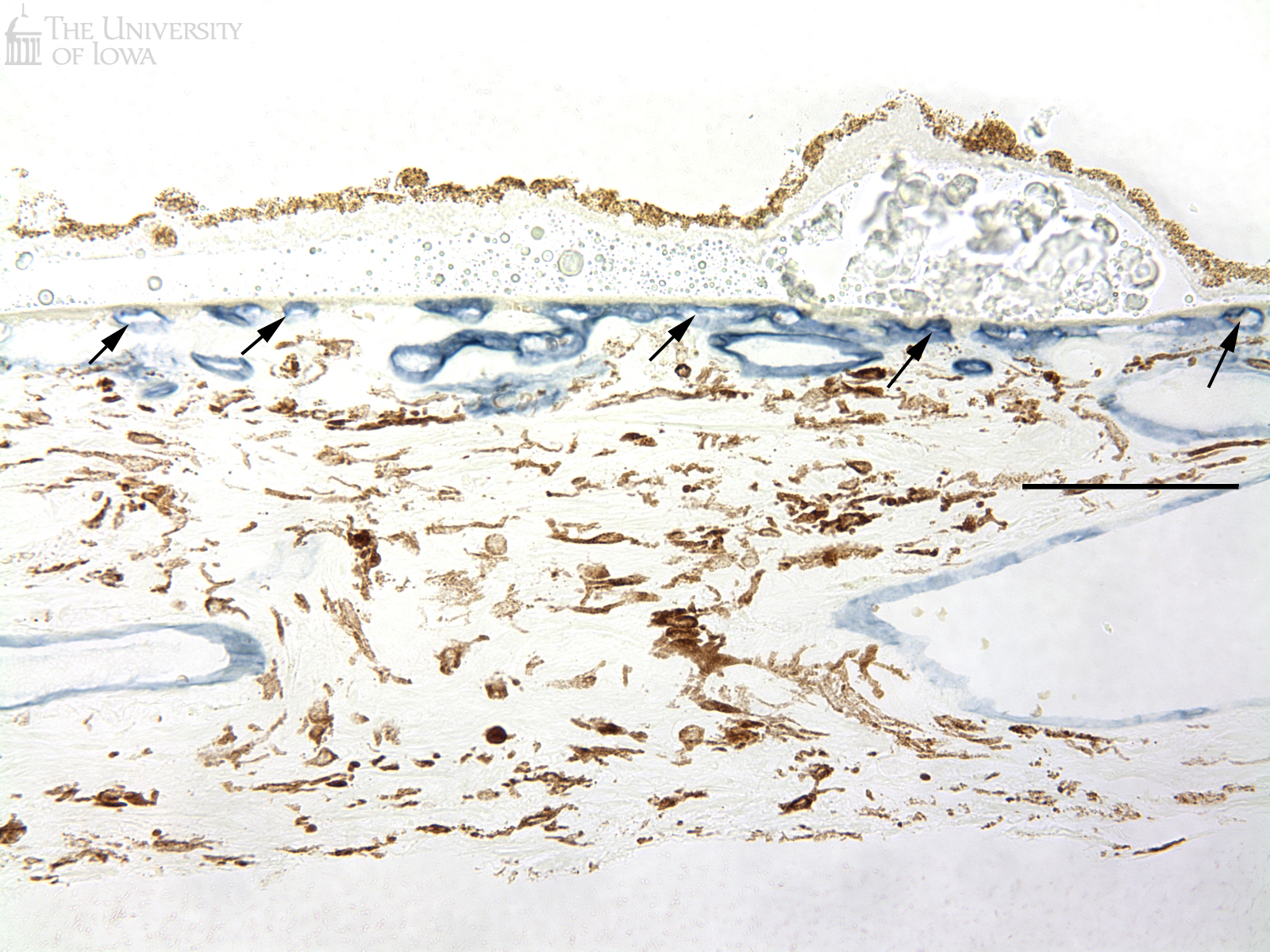
Figure 5 depicts staining of the vasculature (purple) beneath drusen (F) and in an area of scarring from the other eye (G). Viable endothelial cells stain purple with the alkaline phosphatase substrates nitroblue tetrazolium (NBT) and 5-bromo-4-chloro-3'-indolyphosphate p-toluidine (BCIP) under alkaline conditions. Interestingly, while the choriocapillaris persists at least to a certain degree beneath large and diffuse drusen/basal deposits, in areas of scarring from the other eye, only "ghost" vessels remain (i.e., areas resembling capillaries but without viable endothelium, arrows Figure 5B). Vessels in the deeper choroid are viable, however, since they are less reliant on the RPE for their differentiation and viability.
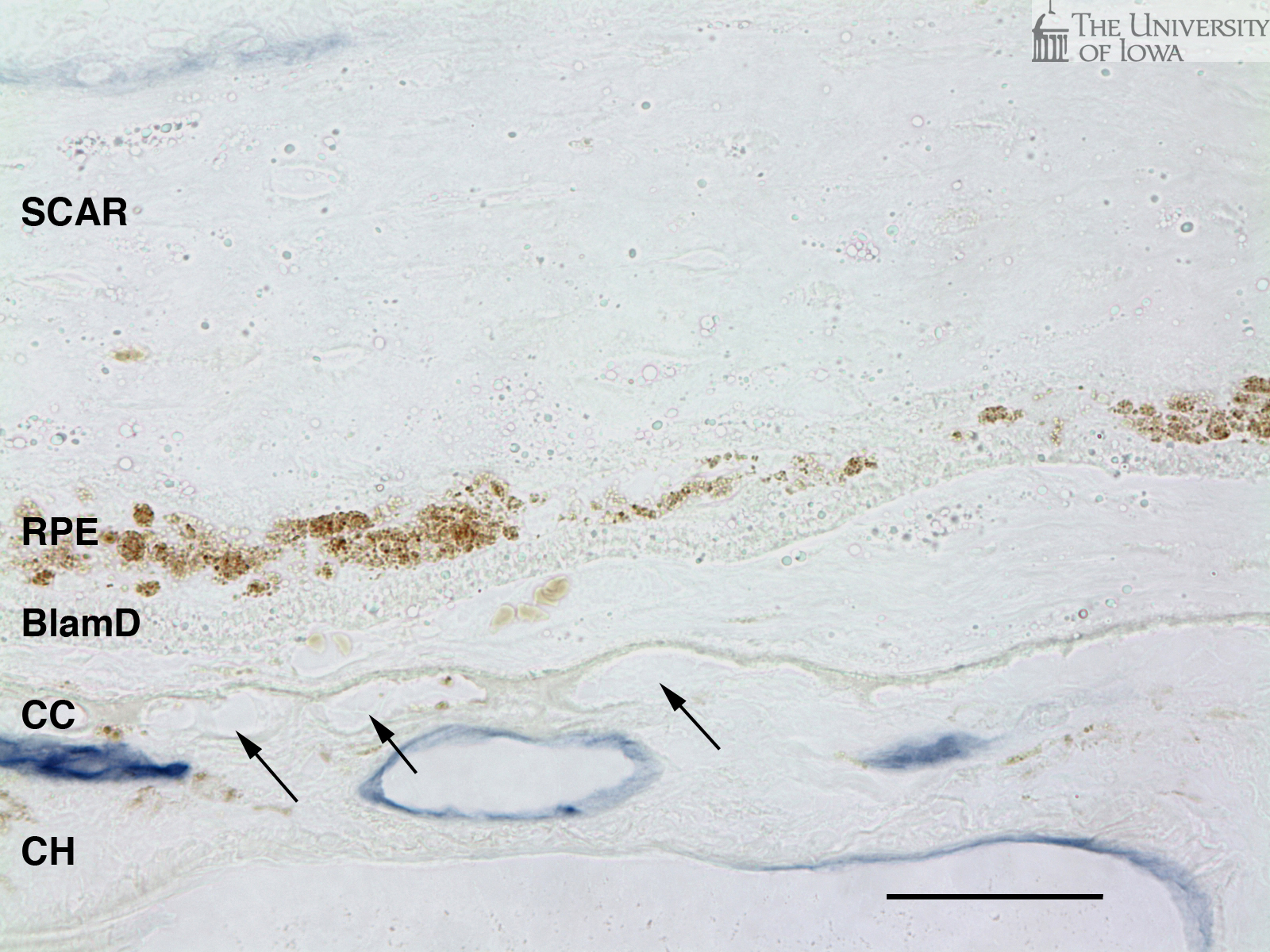
Note Scale: The scale bar is 100µm (Figures 1, 3, 4, and 5A) or 50 um (Figures 2 and 5B) in length. Abbreviations: NFL, nerve fiber layer; GCL, ganglion cell layer; INL, inner nuclear layer; ONL, outer nuclear layer; IS, inner segments; OS, outer segments; RPE, retinal pigment epithelium; CC, choriocapillaris; CH, deeper choroid (Haller’s and Sattler’s layers); NR, neural retina.
Diagnosis: Age-Related Macular Degeneration with drusen
Faidley EA, Skeie JM, Mullins RF. Age-related macular degeneration/age-related maculopathy: a histopathologic analysis. EyeRounds.org. Feb 15, 2008; available from https://eyerounds.org/tutorials/drusen/